Home > Press > Nanometer-Scale Growth of Cone Cells Tracked in Living Human Eye
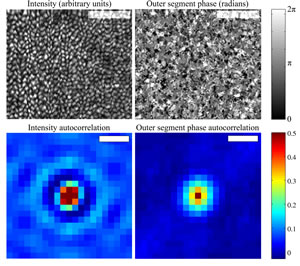 |
| Upper left) En face projection of the cone mosaic, produced by co-adding intensity from the inner segment outer segment junction (ISOS) and outer segment posterior tip (PT) layers, segmented from a single AO-OCT volume. The bright spots correspond to individual cones. Each cone is ~5 μm in diameter. Scale bar 50 μm.
(Upper right) En face projection of the outer segment referenced phase, created by subtracting the phase at ISOS from the phase at PT. Phase correlation is apparent, at a scale similar to that of the intensity projection. Scale bar 50 μm.
(Lower left) Autocorrelation of the intensity projection, possessing the stereotypical appearance of a uniformly packed mosaic. The distance between concentric peaks agrees with the predicted cone row spacing. Scale bar 5 μm.
(Lower right) Autocorrelation of the referenced phase projection, lacking the concentric rings observed in the intensity autocorrelation. Scale bar 5 μm. The similarity between autocorrelations' central peaks suggests that both intensity and phase are correlated among pixels within the cone, while the dissimilarity between the tails suggests that periodicity exists in the intensity image but not in the phase image. Credit: Ravi Jonnal, Indiana University. |
Abstract:
Humans see color thanks to cone cells, specialized light-sensing neurons located in the retina along the inner surface of the eyeball. The actual light-sensing section of these cells is called the outer segment, which is made up of a series of stacked discs, each about 30 nanometers (billionths of a meter) thick. This appendage goes through daily changes in length. Scientists believe that a better understanding of how and why the outer segment grows and shrinks will help medical researchers identify potential retinal problems. But the methods usually used to image the living human eye are not sensitive enough to measure these miniscule changes. Now, vision scientists at Indiana University in Bloomington have come up with a novel way to make the measurements in a living human retina by using information hidden within a commonly used technique called optical coherence tomography (OCT). They discuss their results in the Optical Society's (OSA) open-access journal Biomedical Optics Express.
Nanometer-Scale Growth of Cone Cells Tracked in Living Human Eye
Washington, DC | Posted on December 20th, 2011To make an OCT scan of the retina, a beam of light is split into two. One beam scatters off the retina while the other is preserved as a reference. The light waves begin in synch, or in phase, with each other; when the beams are reunited, they are out of phase, due to the scattering beam's interactions with retinal cells. Scientists can use this phase information to procure a precise measurement of a sample's position. But since in this case their samples were attached to live subjects, the researchers had to adapt these typical phase techniques to counteract any movements that the subjects' eyes might insert into the data.
Instead of measuring the phase of a single interference pattern, the researchers measured phase differences between patterns originating from two reference points within the retinal cells: the top and bottom of the outer segment. The team used this hidden phase information to measure microscopic changes in hundreds of cones, over a matter of hours, in two test subjects with normal vision. Researchers found they could resolve the changes in length down to about 45 nanometers, which is just slightly longer than the thickness of a single one of the stacked discs that make up the outer segment. The work shows that the outer segments of the cone cells grow at a rate of about 150 nanometers per hour, which is about 30 times faster than the growth rate of a human hair.
####
For more information, please click here
Contacts:
Angela Stark
202.416.1443
Copyright © The Optical Society
If you have a comment, please Contact us.Issuers of news releases, not 7th Wave, Inc. or Nanotechnology Now, are solely responsible for the accuracy of the content.
| Related Links |
| Related News Press |
News and information
![]() Simulating magnetization in a Heisenberg quantum spin chain April 5th, 2024
Simulating magnetization in a Heisenberg quantum spin chain April 5th, 2024
![]() NRL charters Navy�s quantum inertial navigation path to reduce drift April 5th, 2024
NRL charters Navy�s quantum inertial navigation path to reduce drift April 5th, 2024
![]() Discovery points path to flash-like memory for storing qubits: Rice find could hasten development of nonvolatile quantum memory April 5th, 2024
Discovery points path to flash-like memory for storing qubits: Rice find could hasten development of nonvolatile quantum memory April 5th, 2024
Imaging
![]() Nanoscale CL thermometry with lanthanide-doped heavy-metal oxide in TEM March 8th, 2024
Nanoscale CL thermometry with lanthanide-doped heavy-metal oxide in TEM March 8th, 2024
![]() The USTC realizes In situ electron paramagnetic resonance spectroscopy using single nanodiamond sensors November 3rd, 2023
The USTC realizes In situ electron paramagnetic resonance spectroscopy using single nanodiamond sensors November 3rd, 2023
![]() Observation of left and right at nanoscale with optical force October 6th, 2023
Observation of left and right at nanoscale with optical force October 6th, 2023
Nanomedicine
![]() New micromaterial releases nanoparticles that selectively destroy cancer cells April 5th, 2024
New micromaterial releases nanoparticles that selectively destroy cancer cells April 5th, 2024
![]() Good as gold - improving infectious disease testing with gold nanoparticles April 5th, 2024
Good as gold - improving infectious disease testing with gold nanoparticles April 5th, 2024
![]() Researchers develop artificial building blocks of life March 8th, 2024
Researchers develop artificial building blocks of life March 8th, 2024
Discoveries
![]() Chemical reactions can scramble quantum information as well as black holes April 5th, 2024
Chemical reactions can scramble quantum information as well as black holes April 5th, 2024
![]() New micromaterial releases nanoparticles that selectively destroy cancer cells April 5th, 2024
New micromaterial releases nanoparticles that selectively destroy cancer cells April 5th, 2024
![]() Utilizing palladium for addressing contact issues of buried oxide thin film transistors April 5th, 2024
Utilizing palladium for addressing contact issues of buried oxide thin film transistors April 5th, 2024
Announcements
![]() NRL charters Navy�s quantum inertial navigation path to reduce drift April 5th, 2024
NRL charters Navy�s quantum inertial navigation path to reduce drift April 5th, 2024
![]() Discovery points path to flash-like memory for storing qubits: Rice find could hasten development of nonvolatile quantum memory April 5th, 2024
Discovery points path to flash-like memory for storing qubits: Rice find could hasten development of nonvolatile quantum memory April 5th, 2024
|
|
||
|
|
||
| The latest news from around the world, FREE | ||
|
|
||
|
|
||
| Premium Products | ||
|
|
||
|
Only the news you want to read!
Learn More |
||
|
|
||
|
Full-service, expert consulting
Learn More |
||
|
|
||








